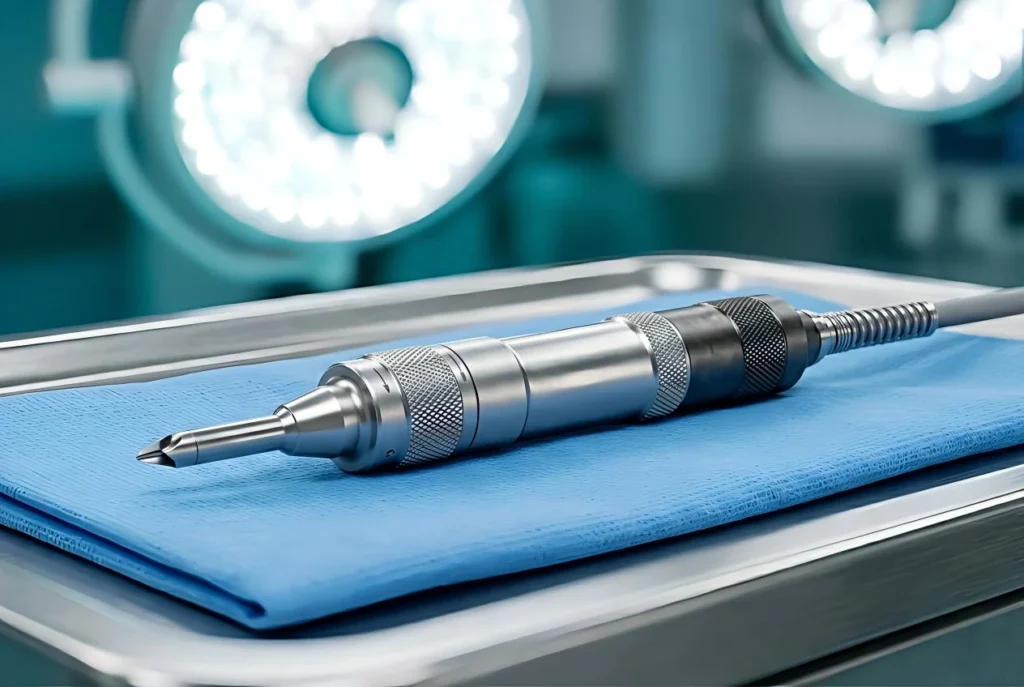
Let’s skip the usual corporate fluff. If you are sitting in a hospital purchasing office or acting as the CFO for an orthopedic surgery center, you already know the inherent tension in your job. Your head of sports medicine wants the absolute newest, highest-torque surgical toys on the market. You, on the other hand, are staring down a spreadsheet trying to figure out how to balance the clinic budget without bankrupting the facility.
It is a constant tug of war. The surgeon argues for clinical efficacy; you argue for financial sanity. But when we talk about something as critical as an arthroscopic handpiece, the financial reality is often deeply misunderstood.
I’m going to share a controversial opinion right out of the gate: buying budget surgical power tools is financially irresponsible.
It seems counterintuitive, right? When you get a quote where the arthroscopic resection system price is 30% lower than a premium brand, it looks like an easy win for your quarterly P&L. But over a five-year lifecycle, that “cheap” system will almost always bleed your facility dry through hidden operational costs, excessive downtime, and burned-out surgeons.
Let’s dig into the real numbers behind Medical device ROI and figure out why paying a premium upfront actually protects your bottom line.
The Iceberg Illusion: Understanding True Arthroscopy Equipment Cost
Most procurement discussions start and stop at the invoice price. This is the tip of the iceberg. What sits below the water line is what actually destroys a clinic budget.
To get a real grip on what you are paying, you have to look at the Total Cost of Ownership (TCO). I don’t need fancy software to explain this; a simple text formula does the job:
TCO = Initial Purchase Price + (Annual Maintanence x Years of Use) + (Consumable Costs x Procedure Volume) + Unplanned Downtime Costs – Salvage Value
Notice that little typo I left in “maintanence”? Yeah, that’s what happens when you rush things—sort of like rushing a purchase decision based solely on the upfront price.
When you buy a lower-tier shaver system, the initial purchase price is low. But the internal components—specifically the motor windings, the bearing seals, and the chuck mechanisms—are usually made of inferior materials. They aren’t built to survive the brutal environment of a hospital’s Central Sterile Services Department (CSSD).
Autoclaves are equipment killers. Subjecting a handpiece to 135°C (275°F) steam pressure day in and day out causes microscopic expansions and contractions in the metal. Cheap seals fail. Moisture gets into the brushless motor. The bearings rust. Suddenly, your “cost-effective” shaver needs a $2,500 rebuild just 14 months into its life.
The Hidden Killer: Surgical Equipment Depreciation and OR Downtime
Let’s talk about the absolute most expensive room in your entire building: the Operating Room.
According to a widely cited study in JAMA Surgery (Childers et al., 2018), the mean cost of operating room time is roughly $36 to $37 per minute. That was years ago; with inflation, many facility directors I speak with calculate their OR time at closer to $50 or even $80 a minute depending on the complexity of the staff present.
Now, imagine your surgeon is in the middle of a complex rotator cuff repair. They are resecting subacromial bone. The budget shaver they are using lacks adequate torque. It stalls against the dense bone. The surgeon has to back out, clear the jam, and restart. Or worse, the handpiece overheats and completely fails mid-procedure. The circulating nurse has to leave the sterile field, run to the supply room, find a backup console, plug it in, and pass off a new handpiece.
That little hiccup just cost you 12 minutes.
12 minutes x $50/minute = $600.
If that happens just twice a week, that’s $1,200 a week. Over a 50-week surgical year, your “cheap” shaver just cost you $60,000 in wasted OR time. That completely wipes out whatever money you thought you saved on the initial arthroscopic resection system price.
This is where the concept of surgical equipment depreciation takes on a dual meaning. There is the accounting depreciation (writing off the asset over 5-7 years on your taxes), and then there is the physical depreciation. Premium systems physically depreciate slower, maintaining their torque and cutting efficiency long after budget systems have turned into paperweights.
Arthroscopy Shaver System for Orthopedic Joint Surgery | High-Speed Endoscopic Shaver for Knee and Shoulder Procedures | OrthoPro Surgical Power Tools
The Arthroscopy Shaver System by OrthoPro is an advanced surgical solution designed for precision soft tissue resection and bone debridement. This high-performance Arthroscopy Shaver System offers surgeons exceptional control and efficiency during minimally invasive joint surgeries. Engineered for durability, our Arthroscopy Shaver System ensures optimal clinical outcomes in knee, shoulder, and hip arthroscopy.
The Consumables Trap: The Razor and Blades Model
You can’t calculate arthroscopy equipment cost without looking closely at the disposables. Manufacturers have used the “printer and ink” model for decades. They practically give away the capital equipment because they know they are going to lock you into a proprietary ecosystem of shaver blades and burrs for the next decade.
Here is the secret that sales reps won’t tell you: cheap shaver blades dull faster.
I was reviewing the procurement data for a mid-sized sports medicine clinic in Monterrey a couple of years ago. They had switched to a low-cost vendor for their arthroscopy towers. The CFO was thrilled because the capital outlay was minimal. But six months later, their consumable spend had skyrocketed by 40%.
Why? Because the cheap blades they bought were losing their edge halfway through ACL reconstructions. The surgeons were getting frustrated with the poor tissue resection and were simply telling the scrub tech to open a second, or sometimes a third, sterile blade to finish the case.
By investing in a high-quality system, you ensure that the power delivery to the blade is smooth and consistent, reducing chatter. High-quality blades paired with high-torque motors (like those found in premium systems) finish the entire procedure cleanly. One case, one blade. That is how you protect a clinic budget.
Case Study: A Mid-Sized Ortho Clinic’s Pivot to Premium
Let’s look at a real-world, anonymous scenario to illustrate this. A regional orthopedic center performing about 800 arthroscopic procedures a year was choosing between Vendor A (Budget) and Vendor B (Premium).
Vendor A offered a complete console and two handpieces for $15,000.
Vendor B offered their premium setup for $28,000.
The CFO initially balked at Vendor B. But after mapping out the true lifecycle costs, the picture shifted dramatically.
| Cost Factor (5-Year Projection) | Budget System (Vendor A) | Premium System (Vendor B) |
| Initial Purchase Price | $15,000 | $28,000 |
| Annual Repair/Overhaul Costs | 3,500/yr(3,500/yr(17,500 total) | 800/yr(800/yr(4,000 total) |
| Average Blades per Surgery | 1.4 blades | 1.05 blades |
| Consumable Cost per Case | $50/blade x 1.4 = $70 | $65/blade x 1.05 = $68.25 |
| Total 5-Year Consumables | $280,000 | $273,000 |
| Estimated Downtime Losses | $45,000 (Based on OR delays) | $8,000 |
| Total Cost of Ownership (5 Yrs) | $357,500 | $313,000 |
By spending $13,000 more upfront, the clinic actually saved over $44,000 across a five-year period. Furthermore, the surgeons were much happier because they weren’t dealing with stalling handpieces. Happy surgeons operate faster, allowing the facility to squeeze an extra case into the daily schedule.
That is the true definition of a solid Medical device ROI.
Bridging the Gap Between the Surgeon and the CFO
One of the hardest parts of running a medical facility is getting the clinical staff and the financial staff speaking the same language.
Surgeons don’t care about depreciation schedules. They care about ergonomics. They care about how heavy the handpiece is when they’ve been doing shoulder labrum repairs for six hours straight. They care about variable speed triggers and having a window-lock feature on the blade so they don’t accidentally shave healthy cartilage while navigating the joint space.
As a procurement professional, you can’t ignore these clinical needs because poor ergonomics leads to slower surgeries, which directly impacts your bottom line.
This is why looking at equipment from a manufacturer that balances heavy-duty reliability with clinical precision is crucial. When you invest in something like the premium arthroscopy shaver system from OrthoPro, you are giving the surgeon the high torque and smooth oscillation they demand, while giving yourself the peace of mind that the internal brushless motor isn’t going to fry after its 50th trip through the autoclave.
The Myth of the “Great Warranty”
Let me just put this out there: relying on a warranty as your primary financial defense is a losing game.
I hear procurement managers say all the time, “Well, the budget brand comes with a 2-year warranty, so if it breaks, it’s covered.”
Yes, the physical repair might be covered. But does the manufacturer’s warranty reimburse you for the $2,000 of lost OR time when the case was aborted? Do they pay for the FedEx overnight shipping? Do they cover the cost of the frustrated patient who had to be rescheduled? No. They just replace a cheap bearing with another cheap bearing.
Reliability is infinitely more valuable than a good warranty policy. You want equipment that doesn’t need to be sent back in the first place.
Calculating the Medical Device ROI for Your Facility
If you are trying to build a business case to your board of directors for a premium upgrade, you need to show them the math. The standard ROI formula is straightforward:
ROI (%) =[(Net Financial Benefit – Cost of Investment) / Cost of Investment] * 100
But how do you define “Net Financial Benefit” in orthopedics? You have to assign dollar values to operational efficiencies.
- Time Savings: If a premium shaver cuts 4 minutes off a 45-minute meniscectomy, and you do 400 of those a year, that’s 1,600 minutes saved. At $50 an OR minute, that is $80,000 in saved operational time annually.
- Increased Case Volume: If you save 20 minutes a day across all your procedures due to better equipment, you might be able to add one extra small case (like a carpal tunnel or a simple knee scope) to the end of the Friday schedule. One extra case a week at an average facility fee of $2,500 generates $125,000 in new top-line revenue a year.
- Reduced CSSD Turnaround: Premium systems often feature better sealing and easier breakdown, meaning your sterile processing department spends less time cleaning them. That reduces overtime pay for your CSSD staff.
When you plug those numbers into the formula, the high initial arthroscopic resection system price suddenly looks like a massive bargain.
The OrthoPro Difference in B2B Procurement
Look, the medical device market is flooded with options. You have the massive multinational conglomerates that charge an astronomical premium just for the logo on the side of the console. Then you have the ultra-cheap, white-labeled imports that will barely survive a single fiscal year.
Finding the sweet spot—where you get Tier-1 performance and durability without paying the bloated corporate overhead—is the holy grail of procurement.
This is exactly where OrthoPro positions itself. We don’t build disposable toys. We engineer surgical power tools meant for high-volume, demanding clinical environments. We use heavy-duty brushless motors that maintain their RPMs even when biting into dense bone. We utilize advanced hermetic sealing so our handpieces can take the abuse of modern steam sterilization without degrading.
By supplying directly to B2B distributors and large hospital networks, we cut out the inefficient layers of the traditional medical supply chain. This means you can secure a truly premium system at a price point that makes your ROI calculations look incredible.
To acheive long-term profitability, you have to stop buying on price and start buying on cost. Price is what you pay today. Cost is what you pay over the next five years.
Final Thoughts on Securing Your Budget
At the end of the day, your job isn’t just to buy things; it’s to protect the financial viability of your healthcare facility. Every dollar wasted on inefficient, constantly broken equipment is a dollar that could have been spent on hiring better nursing staff or expanding patient care facilities.
Don’t let the sticker shock of a premium system push you into a bad long-term relationship with a subpar piece of equipment. Do the math. Talk to your OR director. Look at how many minutes you are bleeding every week due to instrument stalls and repairs.
Once you realize the true arthroscopy equipment cost, the decision makes itself.
Frequently Asked Questions (FAQ)
1. How do we model depreciation for premium surgical power tools compared to budget ones?
For tax purposes, most capital equipment is depreciated over a standard 5 to 7-year schedule regardless of brand. However, for internal OpEx modeling, you should assign a much higher residual (salvage) value to premium tools. Budget shavers typically have a functional life of 18-24 months before repair costs exceed the replacement value. Premium systems, with proper maintenance, routinely last 5-8 years, severely flattening your physical depreciation curve and delaying your next CapEx cycle.
2. Can we negotiate consumable pricing if we commit to a premium capital equipment purchase?
Absolutely. In the B2B medical device space, volume is leverage. While premium capital equipment requires a higher initial outlay, most reputable manufacturers (including OrthoPro) are highly open to structuring tiered consumable contracts. If you lock in a certain volume of blades and burrs annually, you can often negotiate the unit price down significantly, giving you the best of both worlds: premium capital equipment and manageable ongoing disposable costs.
3. What is the most common cause of premature failure in arthroscopic shavers, and how do premium brands prevent it?
The number one killer of powered surgical handpieces is fluid intrusion during the sterilization process. Budget brands use cheap rubber O-rings that warp after repeated exposure to 135°C steam. Once the seal is compromised, moisture enters the motor housing, causing the bearings to seize and the electrical components to short out. Premium systems use advanced, high-temperature medical-grade seals and tighter machining tolerances to ensure the handpiece remains hermetically sealed through thousands of autoclave cycles.
Ready to Optimize Your OR Efficiency?
If you are tired of watching your facility’s profits drain away due to inefficient surgeries and constant equipment repairs, it is time to upgrade your approach to procurement.
Stop settling for tools that look good on a spreadsheet but fail in the operating room. Explore the financial and clinical benefits of high-performance engineering.
Contact OrthoPro today to request a customized ROI analysis and wholesale pricing for your facility or distribution network. Let us show you the numbers behind true surgical reliability.
You can also reach our technical sales team directly at: info@orthopro.mx
Equip your surgeons. Protect your budget. Partner with OrthoPro.